Sometimes medicines, lifestyle changes, or minor office procedures aren’t enough to fix what’s going on. When that happens, surgery steps in and these days, for most gynecological conditions, that surgery means laparoscopy. Tiny cuts instead of one big opening, a camera guiding everything, and tools that let us work with precision. It’s changed the game: far less pain after the operation, much shorter time in the hospital, faster bounce-back to normal days, and scars you can barely see later. That’s why it’s now the go-to method for so many issues, it gets the job done properly while being kinder to the body.
How the Procedure Actually Works
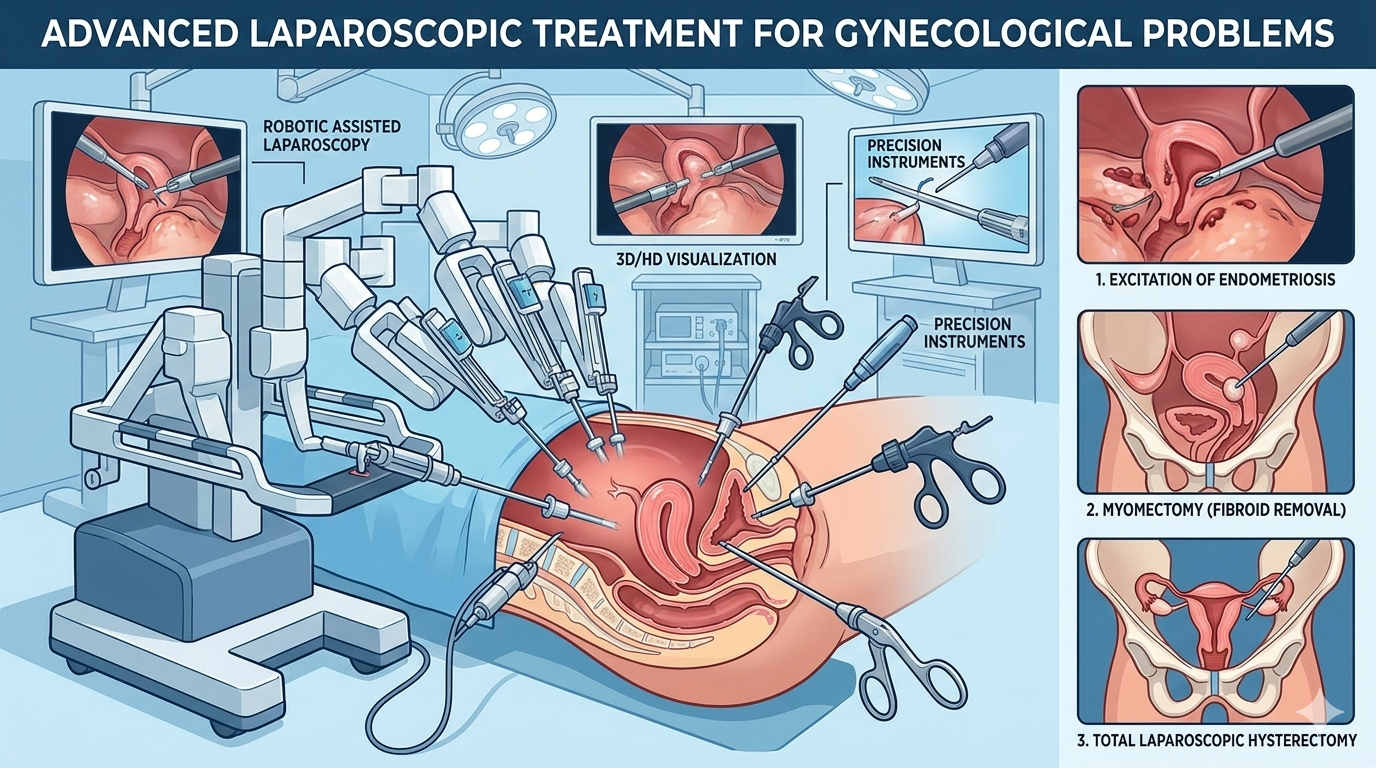
We make a small cut (about 1 cm) near the belly button and slide in the laparoscope—a thin tube with a bright light and high-definition camera. A couple more tiny openings (usually 0.5–1 cm) let us put in the working instruments. Carbon dioxide gas is pumped in gently to lift the abdominal wall away from the organs so we can see clearly. Everything appears magnified on a big screen, and the surgeon uses those fine tools to cut, remove, or repair whatever needs fixing. Once done, the gas comes out, the little cuts get closed with one stitch or surgical glue, and that’s it, no long incision to stitch up or leave a big mark.
Which Problems We Commonly Handle This Way
Endometriosis tops the list. Laparoscopy lets us spot the stray tissue, cut it out, free up any stuck areas (adhesions) that are causing pain or blocking tubes, and sometimes interrupt pain nerves for longer relief. Ovarian cysts, particularly bigger ones or ones that look worrying can be removed or opened and drained without splitting the abdomen open. Fibroids that are messing with the uterus shape or causing heavy bleeding get taken out in a myomectomy, leaving the uterus intact for anyone planning pregnancies later. Blocked or swollen fallopian tubes (hydrosalpinx) can be cleared or removed to boost fertility odds. We also manage ectopic pregnancies safely, perform sterilization by removing or clipping tubes, and clear adhesions or diagnose the cause of long-standing pelvic pain all in the same operation.
Why Most Women Prefer It Over Traditional Open Surgery
The small cuts mean less bleeding during the procedure, lower chance of wound infections, and way less pain afterward. After the first day, most women switch to regular tablets instead of injections or strong narcotics. Hospital time drops to same-day discharge or just one night, compared to 4-7 days with open surgery. Back to light office work in a week or so, full normal life in 3-4 weeks for most. The scars fade to faint lines that disappear under clothes. When the surgeon has plenty of experience, risks like accidental bowel or bladder injury stay very low often lower than with bigger incisions.
Who Usually Does Well with Laparoscopy and When We Might Choose Otherwise
It suits the majority of women who need surgery for the issues above, especially if preserving fertility or avoiding visible scars matters. Younger patients tend to recover quickest. But if there’s a very large mass (say, a uterus stretched like a 5-month pregnancy), dense scarring from lots of previous open operations, or medical conditions that don’t allow safe gas inflation, we might still go the traditional open way. We always go over the options honestly so the plan matches what’s safest and most practical for you.
Before and After: What to Expect
Pre-op checks are straightforward: blood tests, maybe an ECG, and updated imaging (ultrasound or MRI) to map things out. You fast from midnight, get light general anesthesia, and wake up in recovery. That odd shoulder-tip ache from the leftover gas is common but settles fast with walking around and mild pain relief. Mild bloating or period-like cramps happen too. We push gentle movement right away to avoid clots and help the body absorb any remaining gas. Most people head home the same evening or next morning. Follow-up is quick about a week to ten days to look at the cuts and go over what we found and removed.
The Bottom-Line Difference
Advanced laparoscopy isn’t fancy for the sake of being fancy. It’s about reaching the same surgical fix with much less collateral damage to muscles, skin, and recovery time. Women who used to spend weeks flat on their back are now up and moving in days, and the drop in pain and tiredness is huge. When the surgeon does these operations regularly, the results are predictable and safe.
If ongoing pelvic pain, heavy periods that won’t settle, cysts, endometriosis, or fertility roadblocks are part of your story, laparoscopy is frequently the smart next move. If you’re based in or near Delhi and want to see whether it applies to you, you can visit a Gynecologist in Lajpat Nagar New Delhi to talk symptoms through and map out possibilities. Or book an appointment with a Gynecologist in South Delhi to review your scans, ask all the questions, and get a straightforward sense of what the procedure would mean for you. Knowing the facts early takes a lot of the worry out of the decision and usually makes the whole process smoother.