Running a mental health practice today isn’t just about delivering quality care—it’s about navigating a complex financial system that often feels stacked against providers. From fluctuating payer rules to ever-changing coding guidelines, even experienced clinicians can find themselves overwhelmed by the administrative side of care.
That’s where finding the best mental health billing company becomes less of a convenience and more of a strategic decision. The right partner doesn’t just submit claims—they protect your revenue, streamline operations, and allow you to focus on what truly matters: patient outcomes.
But with so many mental health billing companies claiming expertise, how do you separate real value from empty promises?
Let’s break it down.
Why Mental Health Billing Is a Different Game
Mental health billing isn’t identical to general medical billing. It carries its own set of challenges:
- Frequent use of time-based CPT codes
- Nuanced documentation requirements
- Pre-authorization complexities
- Higher claim denial rates for behavioral health services
- Constant payer policy changes
A general billing vendor might handle routine claims well, but mental health insurance billing demands specialization.
Consider a therapist running a growing private practice. They might see 25–30 clients a week, each with different insurance plans. If even a handful of claims are delayed or denied due to incorrect coding or missing documentation, it directly impacts cash flow. Over time, these “small” issues compound into serious revenue leakage.
This is why many providers now look for a mental health billing specialist rather than a generalist.
What Defines the Best Mental Health Billing Company?
Not all billing partners are built the same. The difference lies in depth, not just breadth.
1. Specialization in Behavioral Health
The best mental health billing agency understands psychotherapy codes, telehealth billing nuances, and compliance regulations specific to mental health providers. They don’t treat your practice like a generic clinic.
2. End-to-End Billing Expertise
A true mental health medical billing solution goes beyond claim submission. It includes:
- Insurance verification
- Coding accuracy
- Claims tracking
- Denial management
- Payment posting
Without this full-cycle approach, gaps inevitably appear.
3. Strong Denial Management Process
Denials are not just errors—they are opportunities to recover lost revenue. A capable mental health billing consultant analyzes patterns, identifies root causes, and implements preventive strategies.
4. Transparent Reporting
If you can’t see what’s happening with your revenue, you can’t manage it. The best providers offer real-time dashboards, clear KPIs, and actionable insights.
The Case for Outsourcing: More Than Just Convenience
Many practices hesitate before they outsource mental health billing services. Concerns about cost, control, or communication often come up.
But in reality, outsourcing is often a growth strategy—not an expense.
A Quick Scenario
Imagine a mid-sized therapy group with five clinicians. Initially, they manage billing in-house. As patient volume grows, so do errors:
- Claims submitted late
- Coding inconsistencies
- Increased denials
- Staff burnout
They decide to work with a top outsource mental health billing company. Within three months:
- Claim acceptance rates improve
- Accounts receivable days drop
- Staff can focus on scheduling and patient engagement
- Revenue becomes more predictable
This isn’t unusual. It’s the expected outcome when expertise replaces guesswork.
What to Look for When You Outsource Mental Health Billing Services
Choosing the right partner requires more than comparing pricing.
Experience with Mental Health Providers
Look for a company that has worked specifically with therapists, psychiatrists, and behavioral health clinics—not just hospitals or general practices.
Certified Coding Professionals
A reliable mental health billing and coding company employs certified coders who stay updated with evolving guidelines.
Scalable Systems
Your billing needs today may not match your needs a year from now. The right mental health billing provider grows with your practice.
Compliance and Security
HIPAA compliance is non-negotiable. Your billing partner must ensure data security at every step.
Common Pitfalls Practices Should Avoid
Even experienced providers make mistakes when selecting a billing partner.
Choosing Based on Cost Alone
Low-cost services often mean limited support or lack of expertise. In billing, cheap can become expensive very quickly.
Ignoring Communication Standards
Delayed responses from your billing agency can lead to unresolved issues and missed revenue opportunities.
Overlooking Analytics
Without insights, you’re operating blindly. A professional mental health billing company should provide detailed performance reports.
In-House vs. Outsourced Mental Health Billing
This debate continues across the industry, but the answer depends on your goals.
In-House Billing
Pros:
- Direct control
- Immediate communication
Cons:
- Staffing challenges
- Training costs
- Higher error rates without specialization
Outsourced Mental Health Billing
Pros:
- Access to experts
- Reduced administrative burden
- Improved revenue cycle efficiency
Cons:
- Requires initial onboarding
- Dependence on external partner
For most growing practices, outsourced mental health billing offers more long-term value.
How Billing Impacts Patient Experience
Billing isn’t just a back-office function—it directly affects patients.
Confusing invoices, insurance delays, or unexpected charges can damage trust. On the other hand, smooth billing processes create a better overall experience.
A reliable mental health billing services agency ensures:
- Accurate patient statements
- Timely insurance processing
- Clear communication
When billing runs smoothly, patients are more likely to return and refer others.
Technology’s Role in Modern Mental Health Billing
Today’s leading billing companies leverage advanced tools to improve efficiency:
- Automated claim scrubbing
- AI-driven denial prediction
- Real-time eligibility checks
- Integrated EHR systems
A modern mental health medical billing services outsourcing partner doesn’t just rely on manual processes—they use technology to reduce errors and increase speed.
Signs You Need a Better Billing Partner
If you’re experiencing any of the following, it may be time to switch:
- Rising claim denial rates
- Delayed reimbursements
- Lack of reporting transparency
- Frequent coding errors
- Staff overwhelmed with administrative tasks
These aren’t minor inconveniences—they’re indicators of revenue inefficiency.
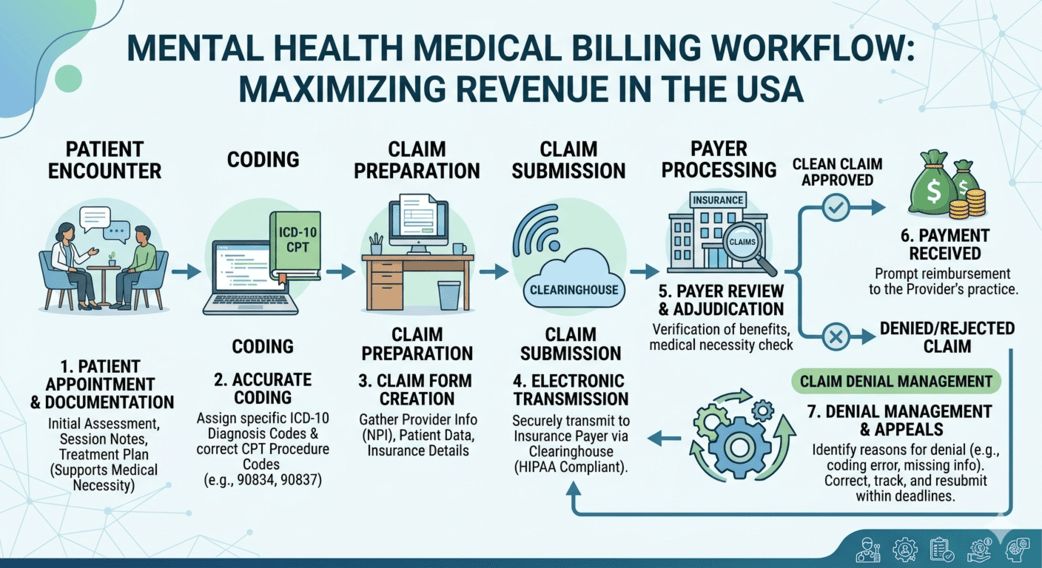
The Bigger Picture: Revenue Cycle Optimization
Billing is just one part of the larger revenue cycle. The best companies understand how each stage connects:
- Patient intake
- Insurance verification
- Coding
- Claim submission
- Payment posting
- Follow-ups
A true mental health billing agency looks at the entire ecosystem, not just isolated tasks.
Making the Right Choice for Your Practice
Selecting the best outsource mental health billing and coding company is ultimately about alignment.
Ask yourself:
- Do they understand my specialty?
- Can they scale with my growth?
- Do they provide measurable results?
- Are they proactive, not reactive?
The right partner becomes an extension of your practice—not just a vendor.
Where Comprehensive Billing Support Fits In
As practices grow, many begin to see the value of integrated support beyond just behavioral health billing. This includes broader medical billing services, accurate medical coding services, and complete medical billing and coding services that ensure consistency across all claims.
Additionally, a strong focus on revenue cycle management helps practices maintain financial stability, while credentialing services ensure providers are properly enrolled with insurance networks—preventing unnecessary delays in reimbursement.
This integrated approach is where providers like 247 Medical Billing Services naturally fit into the conversation. Instead of offering isolated solutions, they bring together multiple aspects of the billing process into one cohesive system, helping practices reduce friction and improve outcomes.
Conclusion: A Strategic Decision, Not Just an Operational One
Choosing the best mental health billing company is not just about outsourcing a task—it’s about strengthening the financial backbone of your practice. The right partner ensures that your hard work translates into consistent, predictable revenue without unnecessary stress.
In a field where time, accuracy, and compliance are critical, relying on experienced professionals can make a measurable difference. From reducing denials to improving patient satisfaction, the impact of a strong billing partner extends far beyond numbers.
As the healthcare landscape continues to evolve, practices that invest in reliable, specialized billing support will be better positioned to grow sustainably. Working with a trusted provider like 247 Medical Billing Services can help bridge the gap between clinical excellence and financial performance—quietly but effectively supporting your long-term success.
FAQs
What makes a mental health billing company different from general billing services?
Mental health billing requires specialized knowledge of psychotherapy codes, time-based billing, and behavioral health regulations, which general billing services may not fully understand.
Is it better to outsource mental health billing?
For many practices, outsourcing improves accuracy, reduces administrative workload, and increases revenue efficiency.
How do mental health billing companies handle claim denials?
They analyze denial reasons, correct errors, resubmit claims, and implement preventive strategies to reduce future denials.
What should I look for in a mental health billing provider?
Look for experience in behavioral health, certified coders, transparent reporting, and strong communication practices.
Can billing services improve patient experience?
Yes, accurate and timely billing reduces confusion, builds trust, and enhances overall patient satisfaction.